Rubella is a contagious, generally mild viral infection that occurs most often in children and young adults. Infection in pregnant women can cause congenital rubella syndrome (CRS) resulting in birth defects of the unborn baby or foetal death.
In children, the disease is usually mild, with symptoms including a rash, low fever (<39°C), nausea and mild conjunctivitis. The rash, which occurs in 50-80% of cases, usually starts on the face and neck before progressing down the body, and lasts 1-3 days. Swollen lymph glands behind the ears and in the neck are the most characteristic clinical feature. Infected adults, more commonly women, may develop arthritis and painful joints that usually last from 3-10 days.
Once a person is infected, the virus spreads throughout the body in about 5-7 days. Symptoms usually appear 2-3 weeks after exposure. The most infectious period is usually 1-5 days after the appearance of the rash.
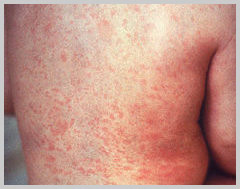
The rubella rash is similar to the measles rash but more pink or light red in colour and spotted.
Rubella virus is transmitted by airborne droplets when infected people sneeze or cough.
Any person with an acute onset of a generalised maculopapular rash and fever 38°C or higher, arthralgia and conjunctivitis.
Rubella PCR on nasopharyngeal swabs is the test of choice. Positive samples are genotyped.
Rubella IgM seroloy is postive from 1-5 days post rash onset.
Positive Rubella IgG with a negative IgM is indicative of either previous vaccination or infection.
Respiratory or other samples collected 7 days before or up to 7 days after the onset of rash from suspected Rubella cases are used for rubella virus detection and strain identification by molecular genotyping.